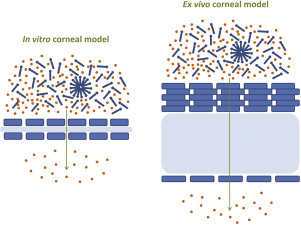
Biopharmaceutical evaluation of surface active ophthalmic excipients using in vitro and ex vivo corneal models
The objective of this study was to systematically investigate the effects of surface active ophthalmic excipients on the corneal permeation of ophthalmic drugs using in vitro(HCE-T cell-based model) and ex vivo (freshly excised porcine cornea) models. The permeation of four ophthalmic drugs (i.e., timolol maleate, chloramphenicol, diclofenac sodium and dexamethasone) across in vitro and ex vivocorneal models was evaluated in the absence and presence of four commonly used surface active ophthalmic excipients (i.e., Polysorbate 80, Tyloxapol, Cremophor® EL and Pluronic® F68). The concentration and self-aggregation-dependent effects of surface active ophthalmic excipients on ophthalmic drug permeability were studied from the concentration region where only dissolved monomer molecules of surface active ophthalmic excipients exist, as well as the concentration region in which aggregates of variable size and dispersion are spontaneously formed. Neither the surface active ophthalmic excipients nor the ophthalmic drugs at all concentrations that were tested significantly affected the barrier properties of both corneal models, as assessed by transepithelial electrical resistance (TEER) monitoring during the permeability experiments. The lowest concentration of all investigated surface active ophthalmic excipients did not significantly affect the ophthalmic drug permeability across both of the corneal models that were used. For three ophthalmic drugs (i.e., chloramphenicol, diclofenac sodium and dexamethasone), depressed in vitro and ex vivo permeability were observed in the concentration range of either Polysorbate 80, Tyloxapol, Cremophor® EL or Pluronic® F68, at which self-aggregation is detected. The effect was the most pronounced for Cremophor® EL (1 and 2%, w/V) and was the least pronounced for Pluronic® F68 (1%, w/V). However, all surface active ophthalmic excipients over the entire concentration range that was tested did not significantly affect the in vitro and ex vivo permeability of timolol maleate, which is the most hydrophilic ophthalmic drug that was investigated. The results of the dynamic light scattering measurements point to the association of ophthalmic drugs with self-aggregates of surface active ophthalmic excipients as the potential mechanism of the observed permeability-depressing effect of surface active ophthalmic excipients. A strong and statistically significant correlation was observed between in vitro and ex vivopermeability of ophthalmic drugs in the presence of surface active ophthalmic excipients, which indicates that the observed permeability-altering effects of surface active ophthalmic excipients were comparable and were mediated by the same mechanism in both corneal models.